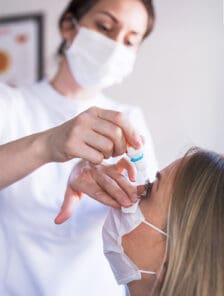
Making Prescription Drugs Affordable
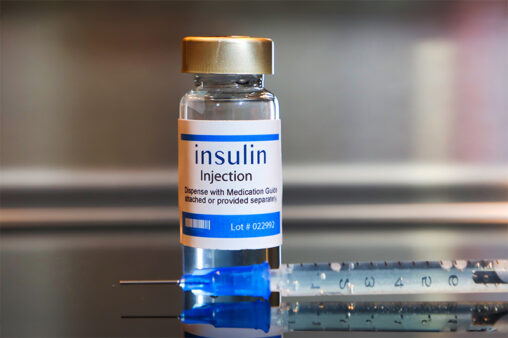
Make prescription drugs more affordable through pricing reforms at state and federal levels.
Expand and protect recent policy actions to lower the price of prescription drugs, including Medicare negotiation.
Increase awareness of the dangers of high-priced drugs to public health.
Reduce financial burden of prescription drugs on older adults.
Americans Support Medicare Negotiation

Despite overwhelming support from everyday Americans, Big Pharma has vowed to fight the Medicare Drug Price Negotiation Program that empowers the agency to negotiate the prices of certain prescription drugs for the first time in history.
The public’s overwhelming support for this policy, even as we head into a presidential election, makes one thing exceedingly clear: people know unfair, anticompetitive behavior when they see it and they want it to stop.
Timothy Lash
President & Chair, West Health Policy Center
A West Health-Gallup public opinion survey shows 83% of Americans favor the program, including 95% of Democrats, 76% of Independents, and 75% of Republicans. Similar levels of support were consistent across age, race, gender, income levels, and education.
Related Resources
Collaborators & Grantees