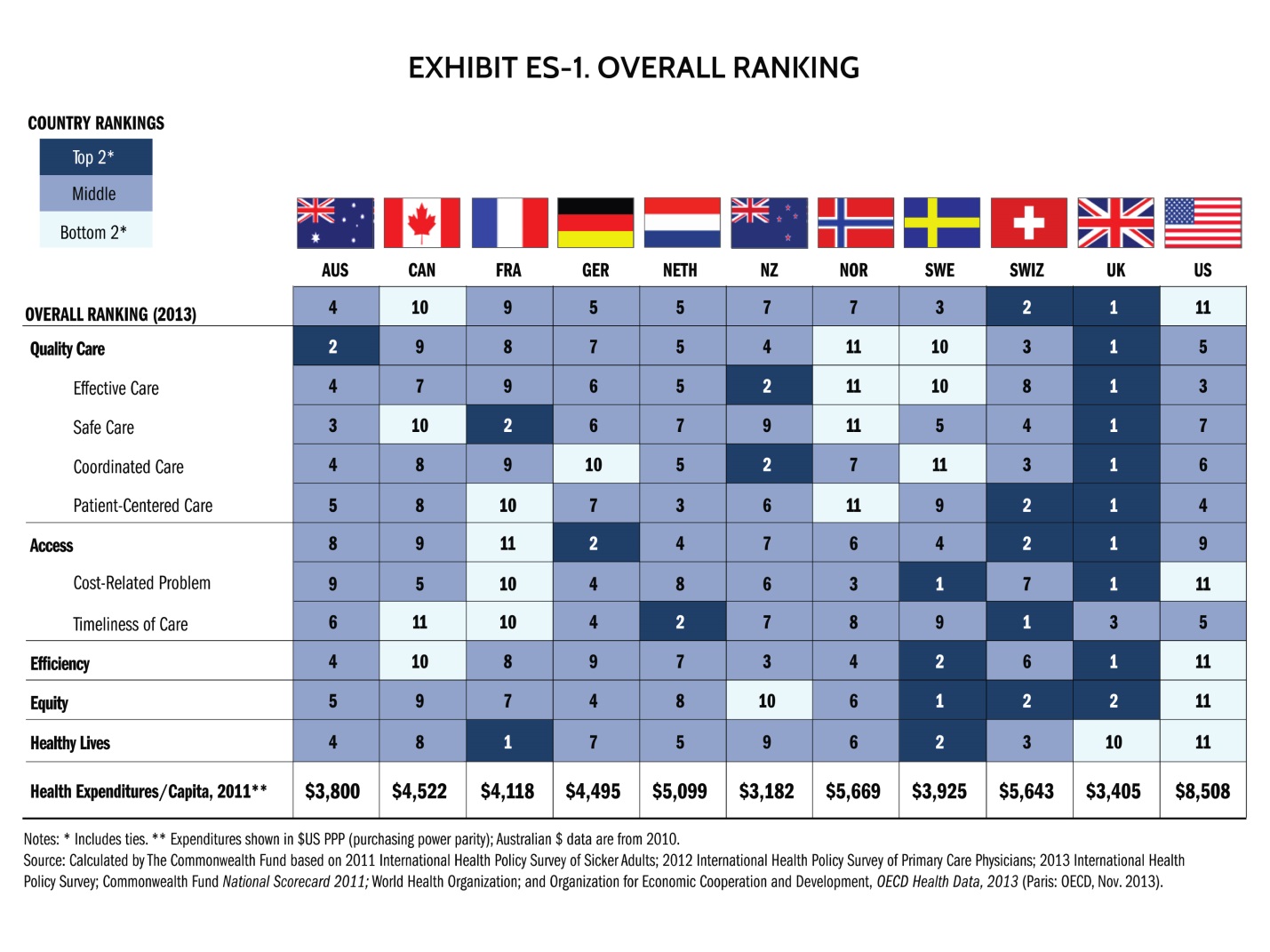
 Everybody loves a winner, and the United States is used to being a global leader on many different economic, financial and business lists. Unfortunately, our position is at the opposite end of the spectrum when it comes to something we should all care about – our healthcare system. In 2010, the Commonwealth Fund’s global look at healthcare among seven leading nations found “the U.S. is last on dimensions of access, patient safety, coordination, efficiency, and equity.” A recently released 2014 update to Commonwealth Fund’s report, Mirror, Mirror on the Wall, 2014 Update: How the U.S. Health Care System Compares Internationally, still ranks the U.S. as last or near last on categories of access, efficiency and equity when compared to 10 other nations.
Everybody loves a winner, and the United States is used to being a global leader on many different economic, financial and business lists. Unfortunately, our position is at the opposite end of the spectrum when it comes to something we should all care about – our healthcare system. In 2010, the Commonwealth Fund’s global look at healthcare among seven leading nations found “the U.S. is last on dimensions of access, patient safety, coordination, efficiency, and equity.” A recently released 2014 update to Commonwealth Fund’s report, Mirror, Mirror on the Wall, 2014 Update: How the U.S. Health Care System Compares Internationally, still ranks the U.S. as last or near last on categories of access, efficiency and equity when compared to 10 other nations.
It’s no secret that the U.S. healthcare system is broken, and that we do poorly when it comes to efficiency and outcomes, especially considering the amount of money we spend. Our country spent approximately $2.8 trillion on healthcare in 2012, about 18 percent of our gross domestic product, outspending, but not outperforming, every other country in the world. Each year we spend more, and as much of a third of this spending is waste that doesn’t improve health, according to the Institute of Medicine. Even more frightening, we are losing a “war on error” in our healthcare system, with errors and resultant harm in hospitals contributing to the deaths of nearly 1,000 people each day in the United States.
Our physicians and patients have difficulty receiving timely information and coordinating care. Caregivers are bogged down by administrative inefficiencies. And as other nations lead in the adoption of modern health information systems, our physicians and hospitals are saddled with inefficient hospital technologies that don’t communicate with each other.
At West Health we are tired of seeing the U.S. healthcare system come in last. We see a light at the end of this tunnel, and it comes from improving our communications in healthcare through medical interoperability, the ability of health information to be shared seamlessly across medical devices and systems.
We’re happy to see and participate in progress on interoperability that could help drive the transformation in our healthcare system for our future.
Earlier this year, we worked with the Office of the National Coordinator for Health IT to draft some key calls-to-action on how everyone in healthcare can help create an automated, connected and coordinated healthcare system that seamlessly shares data – from a patient’s pulse all the way through to a personal, electronic health record that can be accessed in real-time. In June, the ONC launched their 10-year vision with concrete milestones for interoperability, and just last week, the Senate Appropriations Committee demanded a federal inquiry into why, despite billions of dollars having been spent, electronic health records are still not interoperable.
There’s lots of progress still to be made, and I’m confident our nation is on the right track to create an interoperable healthcare system that will help enhance patient safety and improve clinical outcomes at a lower cost.
When the Commonwealth Fund revisits this report four years from now, hopefully there will be references to the impact of medical interoperability and how America is moving towards the top of the list.
